Going the Distance: Innovation in Radiation Research Takes LSU Medical Physics Student from Mary Bird Perkins Cancer Center to SpaceX
April 05, 2021
Jared Taylor was planning on becoming a medical doctor to help treat people with cancer,
but now finds himself almost literally in space, working on solutions to shield astronauts
from dangerous radiation. He recently presented his research at SpaceX and is about
to file a patent.
Students and graduates of the LSU medical and health physics program are changing
oncology, space travel, and more.

Jared Taylor and fellow student Nousha Afshari recently presented their research at SpaceX in California. Graduates from the LSU medical and health physics program find employment in seemingly distant fields (such as space research and cancer care) and are highly sought-after—the placement rate among graduates is 100%. Entrance to the program is also competitive—applicants outnumber those entering the program about nine-fold and tend to hold bachelor’s degrees in physics or nuclear engineering.
– Optional: A photo credit.
Medical and health physics is a specialized field where the laws of physics are applied to medicine and human health. A bit obvious from the name, perhaps, but the applications are wide-ranging. While cancer treatment and space travel would appear to be quite distant from each other, radiation can be the deciding factor between life and death in both areas. It can be used for treatment or diagnosis through medical imaging (X-ray, CT, MRI, ultrasound) as something desirable and useful, but it can also be a threat to people and equipment traveling to the International Space Station, Moon, and Mars, since continuous background radiation in space, beyond the Earth’s protective magnetic field, is one of the hard limits to how much time anyone and anything can spend out there.
“I was thinking of working in a cancer clinic until I joined Dr. Chancellor’s research group and the SpaRTAN Lab at the beginning of last semester, but our program offers a lot of options,” said Jared Taylor, in his third year of the LSU medical physics doctoral program. “Now, I can’t wait to help solve some of the biggest challenges for commercial spaceflight.”
NASA adheres to the recommendation that astronauts should be grounded if their total exposure to radiation, which builds up over time, gives them a 1-in-30 chance of dying from it. But the data scientists use to measure radiation and its effects on people is not always accurate. This is partly because “life in space” is a new thing, and also because we cannot—not ethically and on purpose—expose humans of all different shapes and sizes to radiation, just to see what will happen to them. Much of the research must be done in theory, while some of the data we have on radiation and related health outcomes in practice (such as after the nuclear disasters in Fukushima in 2011 or Chernobyl in 1986), doesn’t translate well; it’s usually from high exposures during a short time instead of low exposures over a longer time.
To get more accurate data, Taylor along with other students in the SpaRTAN (Space Radiation Transport & Applied Nuclear Physics) Lab are developing new models and ground-based space radiation analogs (meaning, environments here on Earth that replicate the complex situation in space—in theory, and in a lab) together with their advisor, Jeffrey Chancellor, assistant professor in the LSU Department of Physics & Astronomy.
One of the students in their research group is Megan Chesal, who is a LaSpace graduate fellow working toward a master’s degree in medical physics with plans for a Ph.D. where her continued research as part of the SpaRTAN group will dive into artificial intelligence and machine learning. Originally from Natchitoches, Louisiana, she is helping the group develop intricate, quite beautiful, and fully digital 3D visualizations of human bodies, called computational phantoms. They can be used to study and predict the biological effects of various types of radiation (different particles and energies) on specific organs, for example. By creating a computerized anatomical man (CAM) and a computerized anatomical female (CAF), Chesal is helping her team see differences in outcomes between men and women. While she got her bachelor’s degree in physics at LSU, her work is now merging with art and biology.
“Our projects influence each other quite a lot,” Chesal said. “Jared is taking my work in new directions while giving me new ideas for mine. It’s a fun feedback loop.”

Jared Taylor
The ultimate goal of the group’s research, of course, is to enable future long-duration spaceflight—perhaps even space colonization. (Chancellor is working on a separate research project with Paul South, assistant professor of plant physiology in the LSU Department of Biological Sciences with a joint position in the LSU AgCenter, on seedlings in space; how we potentially could grow food on spaceships and on the Moon and Mars for future generations.) Chancellor and the SpaRTAN Lab also has three current grants from NASA, totaling over $2.5 million, and two additional grants from LaSpace. (Chancellor has previously provided the go or no-go recommendation for NASA space missions.)
Chancellor and Taylor are currently in the process of filing a patent on technology that uses artificial intelligence to design custom radiation shielding for spacecraft. Their overarching goal, in line with their larger research group, is to develop multiple shielding profiles to help save lives in the design of new space vehicles, but also evaluate the shielding used today on the International Space Station, SpaceX Dragon, and more.
“Given that you only have a certain amount of weight you can bring up there, better shielding is very much an optimization problem,” Taylor said.
Recent advances in 3D-printing technology offer promising new solutions as well.
“It’s about where to put the shielding and how much of it to put where; location and thickness, but also the material itself,” Chancellor explained. “We can now print multiple materials over one solid object in layers. It all depends on where you need the most protection and the least protection. There are instances where you want the radiation to go through because it’s moving fast enough—by adding shielding and slowing it down, you could actually increase your exposure. So, instead of having three or four inches of shielding all over, we’ve developed a way to optimize it for the topography of a particular vehicle.”
SpaceX was the first private company to send astronauts into orbit last year. Visiting the facility in Hawthorne, California last December, Taylor presented his team’s research. With him was also Nousha Afshari, a fellow student in her first year in the medical physics program, intent on a future career in cancer treatment and research. She became all the more motivated to engage in research while working as part of a team that primarily treated cancer patients at the Voice Center in Baton Rouge, housed in the same building as Mary Bird Perkins Cancer Center, before joining LSU.
“I was constantly seeing nearly identical patients who had the same background, lifestyle, cancer in the same location, and the same type of radiation treatment,” Afshari said. “But one would have horrible, chronic side effects while the other would be fine. That just bothered me. Why don’t we know more? Why can’t we give patients better statistics on how the radiation is going to affect them? That’s kind of the driving force behind the research I want to do at LSU. I came into this program with the goal of helping as many people as possible.”
Afshari’s Ph.D. work will build upon some of the findings and outcomes of Taylor’s and Chesal’s projects in producing new ways to predict and understand radiation-induced damage. This will have implications for both space exploration and clinical radiotherapy.
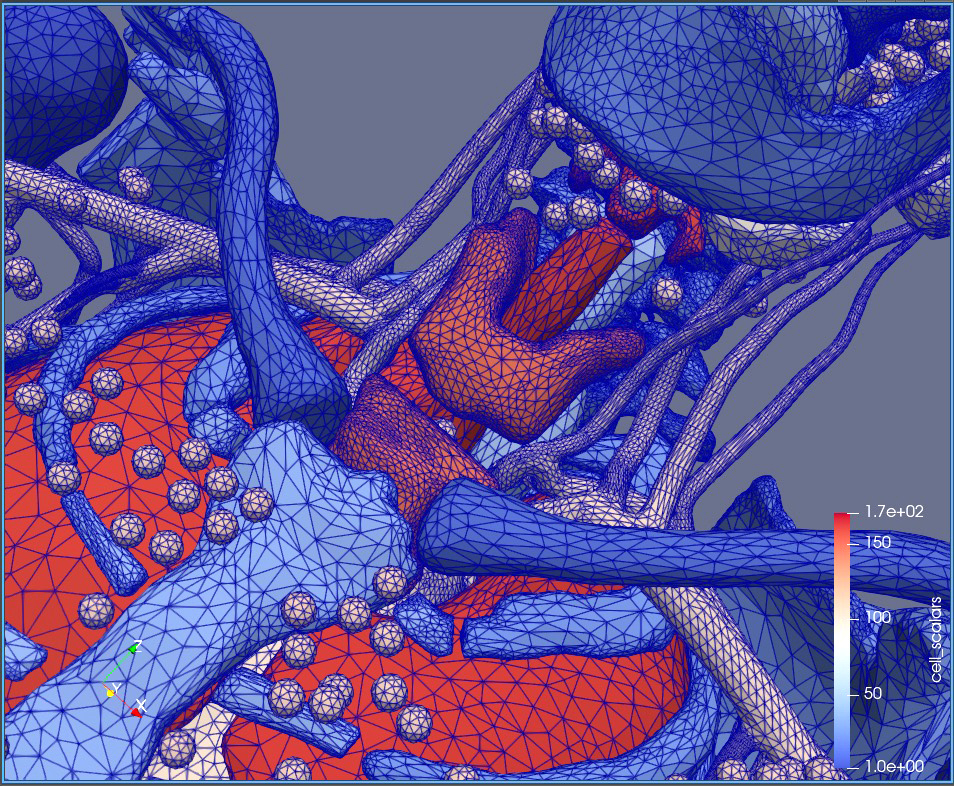
Master’s student Megan Chesal is helping Chancellor’s group develop intricate, quite beautiful, and fully digital 3D visualizations of human bodies, called computational phantoms. They can be used to study and predict the biological effects of various types of radiation (different particles and energies) on specific organs, for example.
LSU and Mary Bird Perkins Cancer Center, a community-owned and not-for-profit care facility, have collaborated closely for decades. The medical physics program at LSU functions as a research arm and on-demand resource to help find answers and solutions to questions and needs that arise in the clinic, while students get hands-on training and occasionally employment at Mary Bird Perkins after they graduate. The clinic’s newest staff member, Christopher Schneider, grew up in Ponchatoula, Louisiana and graduated with a Ph.D. in medical physics from LSU in 2019. He has not yet completed his two-year clinical residency at Mary Bird Perkins, but already accepted an offer for a permanent position.
“We need both scientists and clinicians to help alleviate the burden of cancer; both globally and especially here in Louisiana,” Schneider said. “As a lifelong Louisianan, having a world-class program such as LSU’s right in my backyard has meant everything to me; I found my calling in the medical physics program, and that will allow me to stay here and give back to this state and community that have given me so much.”
The head of the Mary Bird Perkins team, Chief Operating Officer and Chief of Physics Jonas Fontenot, is also an LSU graduate—he added an MBA to his resume last year.
“The LSU-Mary Bird Perkins partnership has become best practice for public-private partnerships with the impact it imparts on student learning and patient care,” Fontenot said. “There are few programs with such robust academic and clinical components to provide the highest level of education to those studying medical physics. Research opportunities with LSU bring a strength to our radiation oncology services that is unmatched in the nation.”
“Meanwhile, the demand for high-quality graduates in this field is intensifying,” he continued. “Many physicists are nearing retirement age, and the general population is getting older and living longer, which means we see more cancer cases. Almost 28,000 people are expected to be diagnosed with cancer in Louisiana this year, and that number is estimated to increase. This is why it’s important that LSU continues to grow and expand its program to provide fully-prepared medical physicists who are ready to serve patients as key members of the oncology team.”
Director of the LSU medical and health physics program, Wayne Newhauser, is proud of its unbeatable job placement rate for graduates, 100%. As president of the national Society of Academic Medical Physics Program Directors, he has a fairly broad perspective.
“We’re very student-focused and students are part of all of the research we do,” Newhauser said. “Students are expected to write up their research and submit to journals and even our master’s students usually have at least one published paper before they leave. Our graduates are highly sought-after, and although it might not be obvious to the average person why space research is lumped in with medical research, we all have to learn the same theories and techniques.”

Meagan Moore (on left) 3D-printed a full-size human phantom for radiation therapy research, called “Marie” (because of radiation researcher Marie Curie and also because her head comes off like Marie Antoinette). Marie is the purple lady on the right, and other than helping with research in labs and clinic, she’s been on display in art galleries. Moore says she enjoys working in what she calls “the maker space” where art meets science.
Collaboration is a big part of the program. Chancellor and Newhauser share two patents; their team member Associate Professor Joyoni Dey was just awarded a new patent on technology to improve breast cancer imaging together with several colleagues in the LSU chemistry department and elsewhere on campus; and they’re continuously recruiting new talent.
Meagan Moore, a current LSU biomedical engineering student and full-time manager of the Andrea Clesi McMakin ’74 STEM Lab at St. Joseph’s Academy (an all-girls Catholic school in Baton Rouge) is considering a Ph.D. in medical physics. She’s been working with Newhauser on several projects already, including 3D-printing a full-size human phantom for radiation therapy research, called “Marie” (because of radiation researcher Marie Curie and also because her head comes off like Marie Antoinette). Moore won 1st place at LSU Discover Day for her poster on Marie and enjoys working in what she calls “the maker space” where art meets science.
More recently, Moore was an integral part of LSU’s PPE production effort for COVID-19, which started in Newhauser’s garage and grew to fill the Pete Maravich Assembly Center, or PMAC. She’s now teaching herself machine learning and is involved in two medical physics projects at LSU; one for the Centers for Disease Control and Prevention (CDC) on better fitting face masks (12 different designs are tested on 5 different face shapes and sizes, each 3D-printed, to see which masks contain more of the breath; a collaboration with the LSU textile department), and one to prevent bruxism, grinding of the teeth. Some of her work is also used in one of Chancellor’s NASA-funded projects.
“I love mashing different technologies together, and medical physics allows me to be extremely innovative with things people don’t necessarily understand,” Moore said. “I love engaging with things that are still unknown.”
For Taylor and Afshari, going to SpaceX to present their research also meant venturing into the unknown.
“Presenting at SpaceX was an opportunity to initiate future collaboration with the company; a chance to present the projects our group is pursuing that would benefit their space exploration efforts,” Afshari said. “We were understandably nervous to present, but the experience resulted in a positive first meeting.”
Taylor agreed:
“It was more of a conversation; they had questions for us and we had questions for them, and they also gave us a tour of the whole facility. We saw the first capsule, the Starlink satellites, and then as we were talking and walking around, we see them building an engine and the people working on it stopped to look up at us. It was a great experience.”
Podcast: A Glowing Interview with Space Radiation Expert Dr. Jeff Chancellor, Part 1 (Space 3D)
LSU physics graduate students invited to present space radiation research at SpaceX (Reveille)
Phantom Project: Moore 3D Prints First Full ‘Human’ for Radiation Therapy Research (LSU College of Engineering)
Where is Cancer Research Headed Next? (LSU College of Science)