Phantom Project
Moore 3D Prints First Full ‘Human’ for Radiation Therapy Research
December 12, 2018
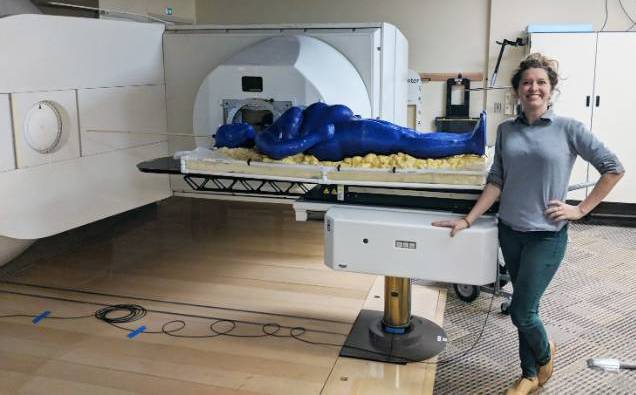 BATON ROUGE, LA – At just 1 year old, she is 5 feet 1 inch tall and weighs 15 pounds.
She can hold 36 gallons of water for up to eight hours. She has a detachable head
but remains faceless. Her name is Marie, and no, this is not her online profile.
BATON ROUGE, LA – At just 1 year old, she is 5 feet 1 inch tall and weighs 15 pounds.
She can hold 36 gallons of water for up to eight hours. She has a detachable head
but remains faceless. Her name is Marie, and no, this is not her online profile.
For the past year, LSU Biological and Agricultural Engineering senior Meagan Moore of Baton Rouge has been working to 3D print the first actual-size “human body” for radiation therapy research. The Phantom Project, also known as Marie, will help test radiation exposure on a real-size human to figure out the best angle for dose distribution.
“Phantoms have been used in medical and health physics for decades as surrogates for human tissue,” Moore said. “The issue is that most dosimetric models are currently made from a standard when people of all body types get cancer. No personalized full-body phantoms currently exist.”
While current phantoms cost $40,000, have no limbs, and don’t represent every body type, Marie represents an entire human body that is more realistic and only costs $500 to create. Using 3D scans of five real women that were procured from the Pennington Biomedical Research Center, Moore developed a lifelike female phantom made of bioplastic that can be filled with water to establish varying density similar to a patient.
“I specifically wanted to work with a woman because, in science, women typically aren’t studied because they’re considered complex due to a variety of reasons,” Moore said. “I want a person with the most complex geometry.”
It took 136 hours to print Marie in four sections on the BigRep printer in LSU’s Atkinson Hall. To connect the sections, Moore used a combination of soldering, friction stir welding, and sandblasting. She even used a hammer and chisel at times to take off chunks of plastic without damaging Marie. The main trouble was figuring out where to put the pipe for dose measurements. It ended up going down the midline from her head to her pelvic floor.
In order to test the phantom on multi-million-dollar equipment, multiple water tests first had to be conducted. During each test, 36 gallons of water were poured into Marie to see if she could hold that weight for 4 1/2 hours. Moore then improvised by using a PVC pipe to catch the “dribbles” that were coming out of some areas.
“This process always makes me nervous, but I know it won’t burst because it has roofing sealant covering it,” Moore said. “The way Marie is shaped also helps.”
Prior to the water testing, Marie was coated with liquid latex and purple roofing sealant for protection. Why purple sealant?
“Purple was on sale,” Moore said. “Turns out the color matches LSU and the University of Washington. She also wears her anti-skid LSU socks.”
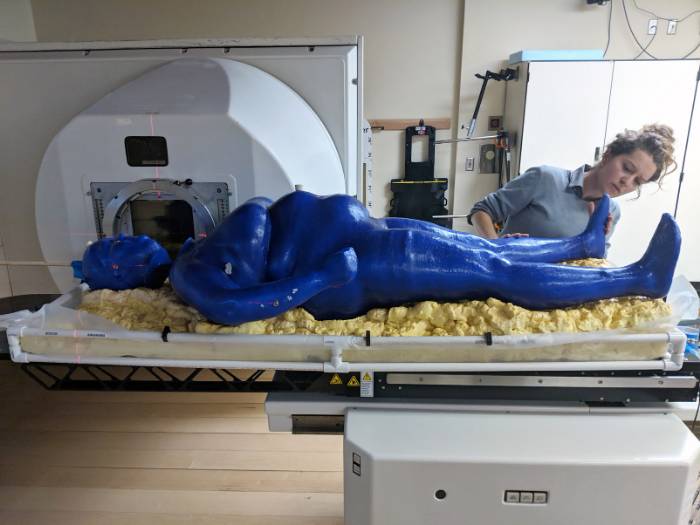 This past October, Moore brought Marie to the UW Medical Cyclotron Facility in Seattle,
where researchers were interested in testing fast neutron therapy on her. This type
of therapy—a specialized and powerful form of external beam radiation therapy—is often
used to treat certain tumors that are radio-resistant, meaning they are extremely
hard to kill using X-ray radiation therapy.
This past October, Moore brought Marie to the UW Medical Cyclotron Facility in Seattle,
where researchers were interested in testing fast neutron therapy on her. This type
of therapy—a specialized and powerful form of external beam radiation therapy—is often
used to treat certain tumors that are radio-resistant, meaning they are extremely
hard to kill using X-ray radiation therapy.
“UW and Oregon Health and Science University came onto the project very recently,” Moore said. “I built a coffin for Marie to get shipped in. I gave workers and handlers a thorough write-up on how to take care of her.”
Marie’s trip was brought about by LSU Medical Physics Program Director and Professor Wayne Newhauser, who not only served as Moore’s mentor on the Phantom Project, but also knew researchers on the West Coast who would be interested in the project.
“The initial idea for the whole project wasn’t completely my idea,” Moore said. “Dr. Becky Carmichael [LSU Communication Across the Curriculum science coordinator and TEDxLSU speaker coach] told Dr. Newhauser that he should talk to me. I met him at his TED Talk, where he did a presentation on 3D printing and how it’s interfacing with science. Since I had just started doing 3D modeling of my own, I showed him my 3D prints. This project took off from his work with breast cancer and computational modeling.
“One reason I like working with Dr. Newhauser is he is good at finding the yes’s,” Moore added. “That’s what pushes each project into existence. Not just having an idea, but the action behind the idea. That’s the kind of environment I like working in, where we can make something happen.”
Art and Science
Moore enrolled at LSU as a BAE student this past fall because she felt the discipline was a platform where she could combine art and science.
“This project started from the art perspective, then became science,” said Moore, who initially wanted to double major in art and science before discovering BAE. “I love talking about the interface between art and engineering because I think it’s really important for how I exist in the realm of science in a lot of ways.”
Moore’s love of science began at a young age, studying fish otoliths with an LSU graduate student while she was in the seventh grade and obsessively attending science fairs.
“I always knew I wanted to do science,” she said. “I was making art with some of the science I was doing and eventually realized I was just tap-dancing around doing engineering. The biomedical engineering environment just kind of came together, and I thought, ‘This is what I’m already doing. This is what I’m supposed to do in life.’
“I created an interdisciplinary role for myself by taking a little bit longer to work on my degree,” she continued. “I’m able to work in a lot of different programs and use a lot of tools. I would love to get a degree and move on, but I learn differently, and if I can share in the process while I’m learning, that’s kind of an incredible setup.”
As for Marie, whose name is a combination of Marie Curie (radiation researcher), Marie Antoinette (detachable head), and Marie Laveau (purple symbolism), Moore hopes personalized replicas of her will be created and used in the medical field to more precisely treat cancer patients.
“What I’d like to see for this project is the research to be used as foundational work to personalize cancer treatments for people with more complex treatments,” Moore said. “Children and breast cancer patients have really differing morphology that is usually very difficult to treat. I find that the more we learn about any body, the more complex it’s going to be. We’re still getting medicine wrong on a lot of levels. We have a lot to learn.”
Like us on Facebook (@lsuengineering) or follow us on Twitter and Instagram (@lsuengineering).
###
Contact: Libby Haydel
Communications Specialist
225-578-5706