In Louisiana, for Louisiana: LSU Fights Rural Health Disparities
April 05, 2021
Across the state, LSU is working to provide more and better healthcare for rural residents.
LSU Health New Orleans has a track for future dentists planning to work in non-metropolitan areas, and its nurse anesthetist program is graduating dozens of certified care providers each year who, in rural hospitals that cannot afford on-site anesthesiologists, are essential to a range of key services, including surgery and childbirth.
LSU Health Shreveport, meanwhile, offers a rare, dual residency for emergency medicine and family medicine—one of only three such residencies in the nation, and ideal for doctors wanting to provide all-in-one care in areas with limited access to other resources—as well as a dedicated rural residency program.
And on LSU’s main campus in Baton Rouge, Professor of Social Work Scott Wilks leads a $3.5 million workforce development effort fueled by federal grants to improve rural access to mental health and behavioral health services in Louisiana, especially among the elderly. Also, through an ongoing collaboration between LSU’s Pennington Biomedical Research Center and the LSU AgCenter, researchers are conducting a five-year study to help explain how two seemingly similar rural Louisiana parishes can have vastly different health outcomes—their goal is to turn new research findings into actionable data for rural communities in all 64 parishes, to help improve residents’ health on their own terms.
Among the top 10 fastest growing (and most needed) occupations in the nation, as many as 6 are in healthcare, according to the U.S. Bureau of Labor Statistics. But not necessarily in large metropolitan hospitals—the need for healthcare is growing just as fast (if not faster) in rural areas, which Louisiana has a lot of (40 among the state’s 64 parishes are classified as rural). This is why the entire LSU Family of Institutions is coming together to educate care providers to help meet the needs of underserved residents.
LSU Health New Orleans (School of Dentistry) Rural Scholars Track

Hannah Broussard chose the Rural Scholars Track at the LSU Health New Orleans School of Dentistry specifically because she wanted to help people in smaller Louisiana communities.
As many as 59 of Louisiana’s 64 parishes are designated as Dental Health Professional Shortage Areas by the Louisiana Department of Health, where the need for care absolutely crunches the supply. To get this designation, a parish must have more than 5,000 potential patients per dentist, which already is a lot considering that any fulltime worker puts in just over 2,000 work hours each year. More than a third of all Louisiana parishes have either no dentist or can count all available providers on one hand. Also, many of the state’s practicing dentists are getting close to retirement age and are predominantly white (only 1 in 10 is Black or Hispanic) and male (3 in 4). Meanwhile, the LSU School of Dentistry in New Orleans is focused on educating not just more dentists, but dentists who are as diverse as the populations they’ll serve. Most of the students are women.
Hannah Broussard from Breaux Bridge, Louisiana (population 8,300) is a third-year student on the LSU Health New Orleans School of Dentistry Rural Scholars Track—a fairly new program established five years ago to help bridge the urban-rural care gap. She’s wanted to be a dentist in a smaller community for as long as she can remember.
“We had like a career day in pre-kindergarten and I told everyone I wanted to be the tooth fairy,” she said. “And because no one wanted to break my heart, they told me that was like a dentist, but I stuck with the tooth fairy for a while until I got older and realized that I really like the sciences.”
While her best friend in the program intends to return to work in her hometown of Franklinton, Louisiana (population 4,000) after they both graduate in May 2022, Broussard isn’t dead set on Breaux Bridge.
“I’ve seen, in my own family, how access to dental care can have a huge effect on quality of life and your confidence and your ability to eat and speak and communicate, and that’s a big part of who we are.”
Hannah Broussard, a third-year student on the LSU Health New Orleans School of Dentistry’s Rural Scholars Track
“As long as I'm in a smaller community, I’ll be happy,” she said. “I’ve seen, in my own family, how access to dental care can have a huge effect on quality of life and your confidence and your ability to eat and speak and communicate, and that’s a big part of who we are.”
Broussard is now refining her skills in extractions, dentures, and crowns, expecting her future patients to need significant amounts of restorative work if they haven’t been able to see a dentist for a long time. Almost half of all Louisianans do not see a dentist on a regular basis, even before the current pandemic.
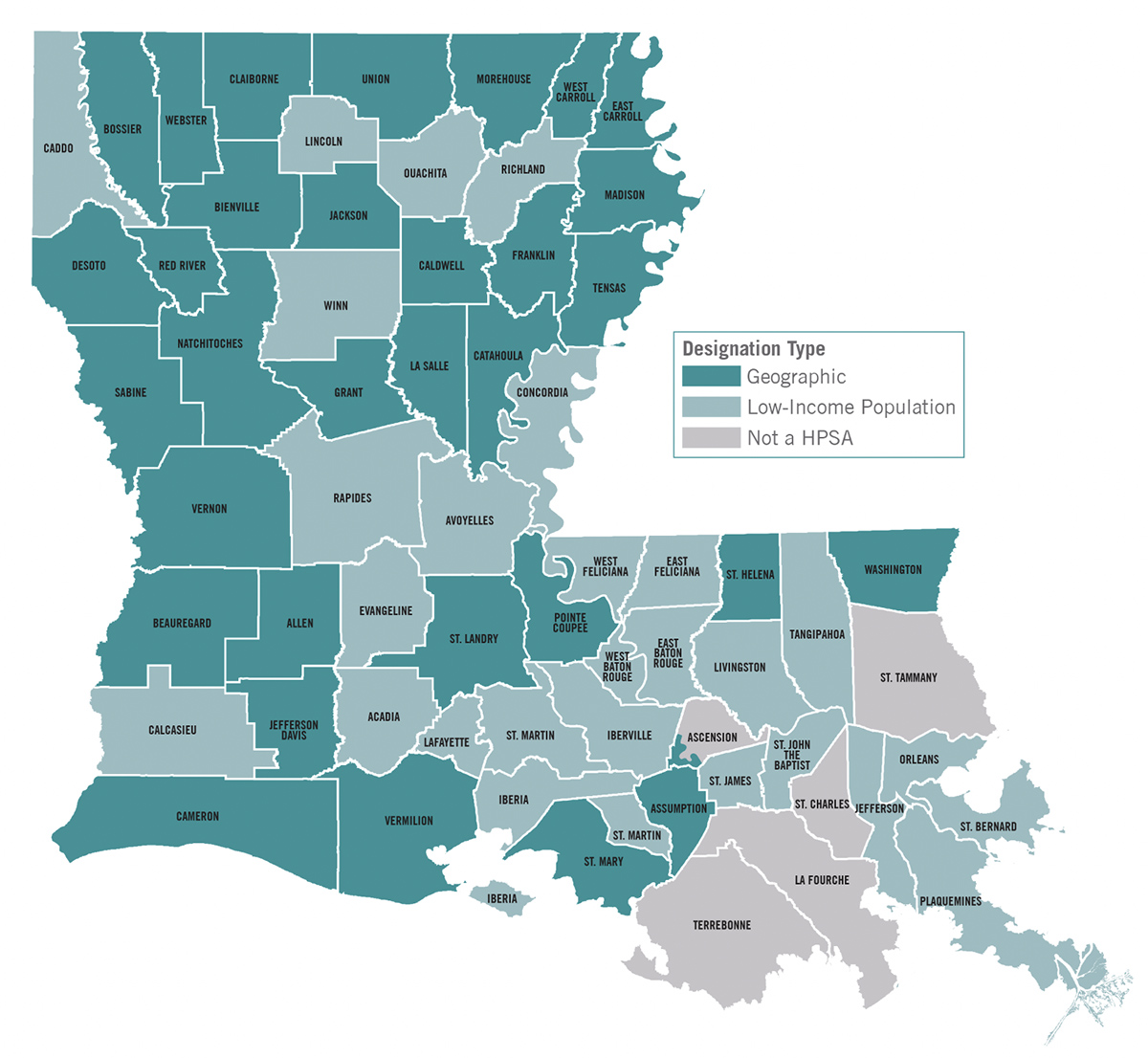
The Louisiana Department of Health has designated 59 of Louisiana’s 64 parishes as Health Professional Shortage Areas for dental care based on geography (not enough dentists) or low-income population (lack of access to existing care). More than a third of all Louisiana parishes have either no dentist or can count all available providers on one hand.
– WellAheadLA.com
“I love the instant gratification, the immediate improvement, the smiles on people’s faces when they see themselves,” Broussard said. “I love being able to interact with people and really get to know them—and as dentists, we can work as part of a team and also have the chance to own our own business. I like working with my hands in an area where science meets artistry.”
Dr. Robert Laughlin, dean of the LSU Health School of Dentistry, would love to see the rural program grow.
“The Rural Scholar Track program will be key to enabling Louisiana to meet its oral healthcare needs in the future,” he said. “The most current dental assessment identified a statewide shortage of at least 200 dentists to serve a population of over 1.8 million. Funding will be paramount for a successful expansion of dental services to all residents of this great state.”
The first Rural Scholars Track graduate, Dr. George “Will” Rolfe, IV, started working in Minden, Louisiana (population 12,000) after completing his training. To reach as many people in need of dentistry as possible, he now combines three jobs, trying to do as much good as he can, including work in the prison system, which takes him east and south to Jonesboro and Monroe on a regular basis.
“I thank God that I love dentistry, because I can work 14 days in a row and it still doesn’t feel like work.”
Dr. George “Will” Rolfe, IV, who began practicing in Minden, Louisiana (population 12,000) after being the first to graduate from the LSU Health New Orleans School of Dentistry’s relatively new Rural Scholars Track
“I thank God that I love dentistry, because I can work 14 days in a row and it still doesn’t feel like work; I just switch from one environment to the other and it’s like a mini vacation,” Rolfe said. “I’m practicing my passion, and I’ve enjoyed working in the prisons a whole lot. It’s really rewarding to be able to immediately restore someone’s self-image and help people sleep easy at night. Also, it’s nice to keep everyone comfortably chewing through all of the good southern food we have down here.”
Another recent graduate of the rural dentistry program, Dr. Anna Womack, began practicing in Vidalia, Louisiana (population 4,000), her home town, last summer.
“I did just about every procedure in dentistry within the first two months,” she wrote to the LSU program coordinator last fall. “Our patient population is very diverse, but we aren’t doing a ton of aesthetic work—it’s more helping people chew again, or getting them out of pain. I’m so thankful I get to do this for the rest of my life!”
LSU Health New Orleans (School of Nursing) Nurse Anesthesia Program
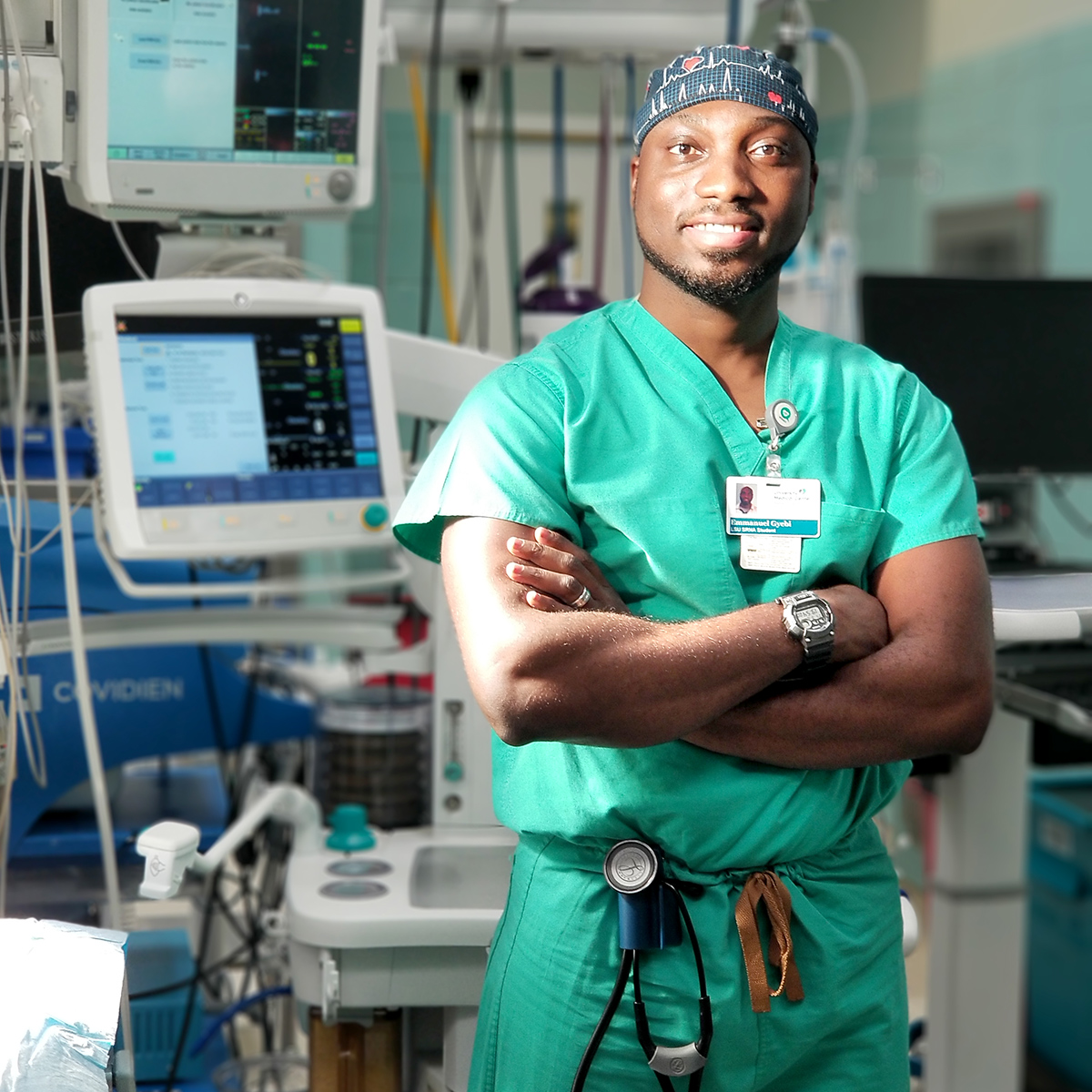
Certified registered nurse anesthetists (CRNA) student Emmanuel Gyebi will graduate from LSU Health New Orleans this May and has already accepted a position to help care for underprivileged and underserved residents.
Certified registered nurse anesthetists (CRNAs) are advanced practice registered nurses and anesthesia professionals who administer more than 50 million anesthetics to patients each year in the United States. In smaller communities and rural hospitals, CRNAs are often the sole anesthesia providers and therefore essential to ensuring access to anesthesia care. In fact, CRNAs represent more than 80% of the anesthesia providers in rural communities. Without them, a hospital like Our Lady of the Angels in Bogalusa, Louisiana (population 12,000) would not be able to perform surgeries or do labor and delivery, for example, saving local residents a long and potentially high-speed and dangerous trip to New Orleans or Baton Rouge.
About 40 new CRNAs graduate each year from the LSU Health New Orleans School of Nursing’s Nurse Anesthesia Program. They must pass a national certification exam and secure licensure as advanced-practice registered nurses. Just this year, the program expanded to take on 60 rather than 50 new students. Meanwhile, this by no means meets demand. Program director Laura Bonanno routinely receives more than 200 applications for these coveted positions, as most (if not all) students find jobs even before they graduate. Last year, as many as 38 among the 41 graduates went to work in what the state calls High Professional Shortage Areas (HPSAs), and the year before, it was 40 of 41. At the same time, all but four parishes in Louisiana are considered primary care HPSAs based on a high ratio of residents per provider or, alternatively, generally low-income populations, meaning the care that’s available isn’t as accessible as the state would like it to be.
“In a rural community such as ours, nurse anesthetists are essential. If not for them, our hospital would not be able to provide the range of services we now do.”
Dr. Richard Karlin, Chief of Surgery at Our Lady of the Angels in Bogalusa, Louisiana
Dr. Richard Karlin, Chief of Surgery at Our Lady of the Angels, appreciates the value CRNAs offer in HPSA parishes.
“At our hospital in Bogalusa, you never know who is coming through the door,” he said. “It can be a woman in labor one minute and a dire surgical emergency the next. Because there is no on-site anesthesiologist, our nurse anesthetists have to be ready for anything—and they are. Also, having LSU Health New Orleans nurse anesthesiology students come work with us is a win-win. They keep us on our toes with their questions; it’s true teamwork, and we hope to expand the program for more students. In a rural community such as ours, nurse anesthetists are essential. If not for them, our hospital would not be able to provide the range of services we now do.”
Raymond Devlin is a CRNA at Our Lady of the Angels as well as part-time faculty at LSU Health New Orleans. He serves as a bridge for the LSU partnership with the local hospital.
“We have LSU students rotate through all the time,” he said. “And not only do we involve them in providing quality care, we’re also making some real changes up here. The major employers in our area is the paper mill and the hospital; we do a lot of indigent and free care, because the population is poor. Washington Parish is also one of the highest opioid abuse parishes in the state, so we jumped on the opioid reduction strategies early on.”
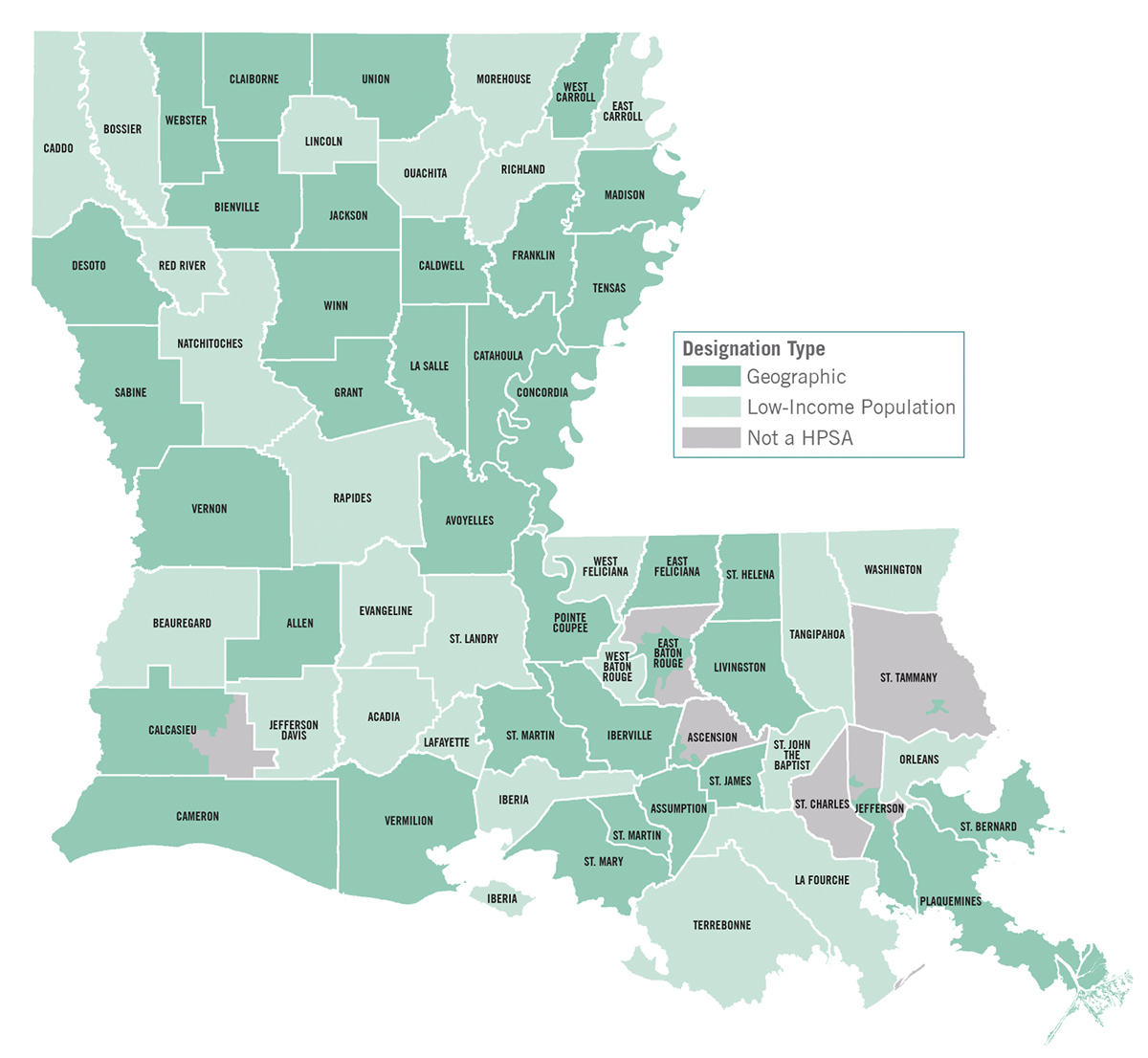
The Louisiana Department of Health has designated 60 of Louisiana’s 64 parishes as majority Health Professional Shortage Areas for primary care based on geography (not enough practitioners) or low-income population (lack of access to existing care). In smaller communities and rural hospitals, nurse anesthetists are often the sole anesthesia providers and therefore key to many essential services, including surgery and labor and delivery. They’re also instrumental in the fight against the opioid epidemic, as they can provide other types of pain management.
– WellAheadLA.com
“That’s where CRNAs really can make a huge difference,” Devlin continued. “We can do regional instead of general anesthesia, as well as epidurals, spinal blocks, and abdominal blocks; ultrasound-guided temporary nerve blocks in different areas of the body, so patients can go home without pain and without oral pain meds and feel fine.”
Last year, Our Lady of the Angels was named a Leapfrog Top Rural Hospital—one of 19 in the nation—and one of 105 Top Hospitals in the U.S. due to its outstanding quality, safety, and forward-thinking care.
Another rural Louisiana hospital, Lallie Kemp Regional Medical Center in Independence, Louisiana (population 2,000) has also partnered with LSU Health, offering clinical rotations for CRNA students. Coordinator and CRNA Bobby Siler describes the experience as an eye-opener for many.
“We take care of some of the sickest people, and lots of people who’ve never been to a doctor before,” he said. “So, when they come in, maybe with a gaping wound, we have no medical history on them; no known allergies, nothing. We have to work them up from scratch on the fly so they can have a procedure and receive anesthesia safely. This means we have to look at their heart, lungs, kidneys, possible coagulation issues—everything, and fast.”
“I wanted the most autonomous position I could have as a nurse, and that’s what put me on the CRNA track.”
Bobby Siler, CRNA at Lallie Kemp Regional Medical Center in Independence, Louisiana and LSU Health New Orleans graduate, whose mother and four sisters also are nurses
Siler graduated from LSU Health New Orleans as a CRNA in 2011 and comes from a family of nurses.
“My mother is a nurse and my four older sisters are nurses,” he said. “Taking care of people is what our family does. Me, I wanted the most autonomous position I could have as a nurse, and that’s what put me on the CRNA track.”
“In my view, we provide excellent and cost-effective care for our community,” Siler continued. “I love taking care of people.”
A current LSU CRNA student set to graduate this May is Emmanuel Gyebi. He’s already accepted a position to help care for underprivileged and underserved residents.
“I chose LSU for its national acclaim in producing exceptionally gifted clinicians who transcend their generation in practice and epitomize the future of healthcare,” Gyebi said. “I look forward to the privilege of being an independent provider adequately trained to meet the anesthetic needs of patients with limited access to quality healthcare.”
LSU Health Shreveport Rural Residency Program, and Dual Emergency Medicine/Family Medicine Residency Program

Danielle Thomas, a current resident in the LSU Health Shreveport rural residency program, sees the value in training where you intend to work, and working where you trained. And since most doctors tend to practice within an hour’s drive of where they did their residency, it’s easy to understand how important it is for underserved communities to have a rural residency program.
– Optional: A photo credit.
Recruiting doctors to work in a rural area can be tricky if they have no experience or history in that place or in any small community. Dr. Luke Baudoin, program director for the LSU Health Shreveport rural family medicine program in Vivian, Louisiana (population 3,600) knows this well.
“We started this program because rural clinics and hospitals in our state were having a difficult time recruiting physicians,” he said. “And among the eight physicians we have on staff in Vivian now, five are actually graduates of our rural residency program.”
Residents who do a clinical rotation in Vivian as part of their training get to work in all aspects of care—clinics, emergency care, inpatient care, as well as specialty care. Students in the rural residency program spend their entire time in their final two years in an underserved, rural area, as opposed to the month-to-month block rotation you’d have in a typical residency.
“Access to healthcare is a major challenge in rural areas, and the need is great,” Baudoin said. “Our average resident sees almost 2,000 patients prior to graduation. This is part of the reason LSU Health Shreveport recently reinvested in our program, so we now have three new residents each year, instead of two. Soon, we’ll have a total of nine.”
One of the current residents is Danielle Thomas, intent on working in the small town of Minden, Louisiana (population 12,000) after she completes her training in Vivian. Originally from a small town in Idaho, Thomas says she “felt in her heart” that Minden would be the right place for her after she spent some time in the community.
“Minden is a beautiful little town, but really suffering in terms of primary care while they do have some specialists,” Thomas said. “When I went to visit, they took me around to every single doctor’s office and they were all really interested in working together.”
“When I got to the West Coast, I just couldn’t believe it; I went to see a doctor and was told, ‘You need to see this other doctor for this, and that other doctor for that,’ and I was like, ‘Why? Why can’t you help me?’”
Danielle Thomas, a resident of the LSU Health Shreveport rural family medicine program, on how she very much prefers the all-in-one “village doctor” approach to care and intends to practice in Minden, Louisiana
Meanwhile, Thomas hopes to offer the kind of all-in-one care she experienced growing up in Idaho, where the family doctor who delivered her then took care of her until she left for college in California.
“When I got to the West Coast, I just couldn’t believe it; I went to see a doctor and was told, ‘You need to see this other doctor for this, and that other doctor for that,’ and I was like, ‘Why? Why can’t you help me?’”
Looking at the rural residency program at LSU Health Shreveport and the small town of Vivian on a map, Thomas wasn’t sure at first. She’d heard bugs in the South could be as big as her head.
“But I came down and the hospital was amazing,” Thomas said. “Although we’re understaffed and it’s been really hard; we work a lot and we’re on call every fourth day, I love that the doctors who work with us trained here, and the bugs really aren’t that bad. There are very few things that scare me now.”

Danielle Handrop is a first-year resident in LSU Health Shreveport’s dual residency five-year program for emergency medicine and family medicine, one of only three such programs in the nation. The program uniquely prepares doctors to be, as Handrop says, “ready for anything” in remote areas where they might be the sole healthcare provider.
Since most doctors tend to practice within an hour’s drive of where they did their residency, it’s easy to understand how important it is for underserved communities to have a rural residency program, Baudoin argues.
“Many underserved residents work in jobs that form the backbone of our economy, such as farming, ranching, and forestry, while others simply cannot afford to live where the big hospitals are. Our goal is to produce competent, caring doctors to help serve these communities since all people need and deserve access.”
Baudoin also oversees the fairly unique LSU Health Shreveport program that combines emergency medicine and family medicine into an extended five-year residency (one of only three in the nation). Although the focus of that program isn’t strictly rural, some of its residents rotate through the North Caddo Medical Center in Vivian, Louisiana and commit early on to practice in rural areas after they pass their final board exam.
Danielle Handrop, a first-year resident, is among them. Combining emergency medicine and family medicine made sense to her because she’d be “ready for anything” in a remote area where she might be the sole healthcare provider.
“That’s what I want, specifically,” Handrop said. “I want my future patients to get all the care they need in one place, through one person, and not have to travel. I want to help grandmas and grandpas and babies—everyone—so having both the emergency and family medicine training was really important to me.”
“I want my future patients to get all the care they need in one place, through one person, and not have to travel.”
Danielle Handrop
Handrop grew up in Blanchard, just northwest of Shreveport, while her husband is from Vivian. Although they currently both work in Shreveport, they “live out in the sticks” and intend to keep it that way, hoping to one day bring their workplace closer to home.
“I knew I wanted to stay here because it’s better for my family and that’s how I was raised,” she said. “I’d love to bring back house calls; we’ve gone away from it in medicine, but I like that culture of care and what it means to be someone’s family doctor, where you still see each other in church and at restaurants. That’s the career I want.”
LSU Health Shreveport also involves additional medical students in primary care for rural and medically underserved communities through the Area Health Education Center, or AHEC, program.
LSU School of Social Work’s Behavior Health Workforce Education and Training (BHWET) Program
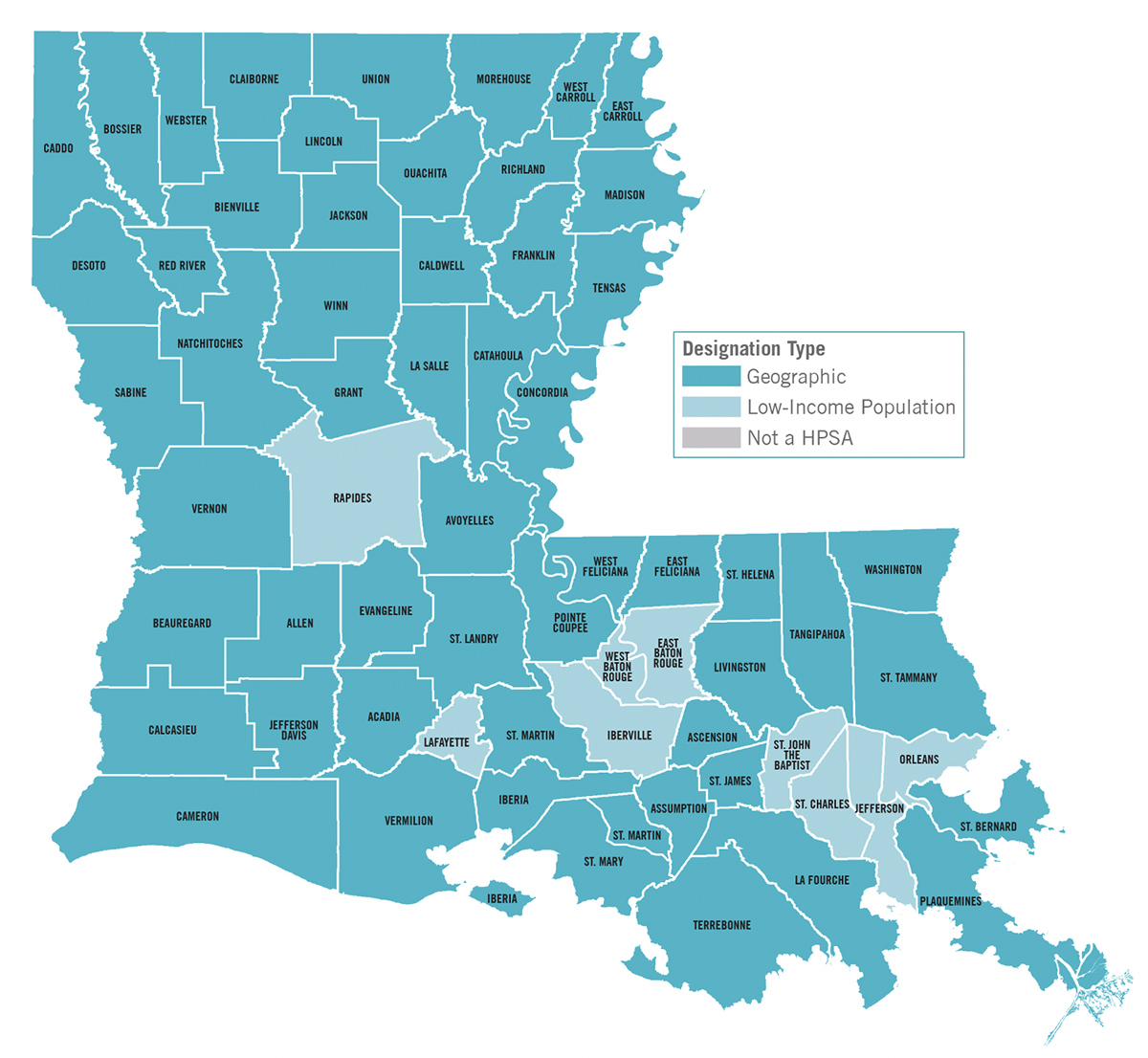
The Louisiana Department of Health has designated all of Louisiana’s 64 parishes as Health Professional Shortage Areas for mental health care based on geography (not enough practitioners) or low-income population (lack of access to existing care).
– WellAheadLA.com
Since 2014, LSU and Professor Scott Wilks have trained over 200 graduate students to help meet behavioral health needs in medically underserved areas in Louisiana through the Behavior Health Workforce Education and Training (BHWET) program, with a total of $3.3 million in support from the Health Resources and Services Administration (HRSA), which is the primary federal agency for improving healthcare for people who are geographically isolated, or economically or medically vulnerable.
A substantial majority of all eligible LSU students (all entering their final year toward their master’s degree in social work) apply for the 30 scholarships available every year. Each of those selected receive $10,000 in support and are placed in a year-long behavior health-related internship anywhere in the state.
“Students often assume we’re going to want them here in Baton Rouge, near the main campus, but that’s not necessarily accurate,” Wilks said. “On the contrary, if they’re in a rural community on the opposite end of Louisiana and would prefer to stay there, that’s great, because we want these students to be committed to living and working where they’re familiar and most needed, including in rural areas.”“There’s still a stigma around mental health, and it seems harder and harder every day to find placement for those who need to go to a facility with qualified, trained staff.”—LSU BHWET scholar Breanna Foster, who is a current behavioral health intern at Lane Regional Medical Center in Zachary, Louisiana
“There’s still a stigma around mental health, and it seems harder and harder every day to find placement for those who need to go to a facility with qualified, trained staff.”
LSU BHWET scholar Breanna Foster, who is a current behavioral health intern at Lane Regional Medical Center in Zachary, Louisiana
The need for mental and behavioral health services is great in Louisiana. Every parish in the state is considered a High Professional Shortage Area (HPSA). And although there are more providers around Baton Rouge, New Orleans, Lafayette, and Alexandria, the care isn’t always accessible for low-income residents.
As interns, BHWET scholars often coordinate with other local health care providers to strive for integrated care for clients who might need behavioral health services to help them cope with stress, depression, substance abuse, or problems that arise from living with a chronic physical health condition. These services can be especially important with the isolation and other challenges brought on by the COVID-19 pandemic.
Scholars also attend training seminars throughout the year to help elevate their skills. Some of those sessions are offered in partnership with Southern University’s Master of Science in Nursing program and address, among other things, how to communicate effectively with diverse populations and non-pharmacological interventions for people with Alzheimer’s disease and related disorders.

Professor Scott Wilks leads the LSU Behavior Health Workforce Education and Training (BHWET) program, which aims to increase and improve behavioral health services for all of Louisiana, including rural areas.
– LSU
“Our goal is to help serve the entire state by elevating our trained behavioral health workforce,” Wilks said. “We have enormous healthcare needs in Louisiana, so it isn’t difficult to convey the need for getting more of our students into the workforce as soon as possible. Meanwhile, no one understands better than the people who grew up in medically underserved rural areas—including many of our students—just how underserved they are.”
“This is something we value as we select scholars for the BHWET program,” Wilks continued. “We ask them during the application and interview process, ‘Understanding that life can quickly change and we can’t predict the future, are your career expectations and intentions to remain in Louisiana and help serve the population we’ll specifically train you to serve?”
Current BHWET intern Breanna Foster answered yes to that question. She is now working at Lane Regional Medical Center in Zachary, Louisiana. Growing up in Central, Louisiana (before it became a city in 2005), Foster didn’t think much about mental health.
“It was a very supportive community; we never locked our doors and if a neighbor needed help, all they had to do was ask,” Foster said. “But mental health was different; a few of my friends died in high school and the guidance counselor was not a friendly woman to go and talk to. So, when I experienced traumas, I had to tackle them on my own. This is why I wanted to be a support for those who need it, if they want it, because there’s still a stigma around mental health, and it seems harder and harder every day to find placement for those who need to go to a facility with qualified, trained staff.”
LSU’s Pennington Biomedical Research Center and LSU AgCenter Collaboration: The RURAL Study

Employees at Assumption Community Hospital take the new walking trail through the park that was established in collaboration with the LSU AgCenter’s Healthy Communities initiative. Residents in Assumption Parish will soon have the opportunity to participate in the new RURAL study, led by LSU’s Pennington Biomedical Research Center in partnership with the LSU AgCenter.
– Olivia McClure
Two seemingly similar Louisiana parishes in terms of demographics, Assumption and Franklin, have vastly different bills of health. While mortality rates from heart, lung, blood, and sleep disorders are 20% lower in Assumption compared to the national average—thus, significantly better—mortality rates in Franklin are 70% higher. It’s a stunning difference that’s difficult to explain. Even once adjusted for poverty (19% versus 26%), the disparities are stark.
“Although they’re a near match for demographics, they have very different disease rates,” said Stephanie Broyles, lead Louisiana investigator of the ongoing National Institutes of Health (NIH)-sponsored RURAL study. “This was curious, and how we got started.”
RURAL stands for Risk Underlying Rural Areas Longitudinal. It’s the first long-term study to look at health disparities in rural parishes and counties compared to each other rather than urban-rural differences.
“This is a deep dive into rural health to try to better understand the drivers of disease,” Broyles said. “What we hope to discover, too, are factors that are important for health in rural areas but may not be important in urban areas. We’re looking at rural health on its own terms, whether the factors are part of the built environment or the social environment or something else.”
By figuring out why residents in some rural parishes and counties in the South live long and healthy lives, the researchers hope to identify solutions that could help residents in other areas. Beyond nearly 800 people in the two parishes in Louisiana, the study will follow about 3,800 in eight rural counties in Alabama, Mississippi, and Kentucky for as long as they wish to be part of the study. The next four years will be spent recruiting participants and gathering baseline data. And for this purpose, researchers will be traveling around the South with a clinic on wheels, outfitted with state-of-the-art equipment.
“We’re hoping to use this study as an opportunity to link underserved communities with care.”
Stephanie Broyles, lead Louisiana investigator of the RURAL study
“We wanted to make sure people’s ability to travel to the study site wasn’t going to be a speed bump in anyone’s participation,” Broyles said. “We want a true cross-section of the population, including people who might not have ever been to see a doctor before. We’re hoping to use this study as an opportunity to link underserved communities with care.”
Broyles expects there to be incidental findings, also. This is because she was part of a Healthy Communities health assessment in West Carroll Parish a few years ago where several residents discovered, through the study, that they had diabetes, high blood pressure, or high cholesterol.

Part of the LSU AgCenter’s Healthy Communities initiative is to work with local schools to establish and run gardens. Here, young hands check on a young broccoli at Choudrant Elementary in Lincoln Parish. Healthy Communities will play an important role in disseminating the findings of the RURAL study to all Louisiana communities, and working together to implement any changes rural residents would like to make.
– Cathy Judd
While the results of the four-state study won’t be compiled and published until 2025 or later, Broyles is eager to share whatever the Louisiana component of the study will find with local residents as soon as possible. By collaborating with the Healthy Communities initiative run through the LSU AgCenter with lead Denise Holston and extension agents on the ground in every Louisiana parish, Broyles hopes to be able to use the study to connect rural communities with research, help answer questions local residents might have, and work with residents to implement changes they want to see in their areas—something Healthy Communities already is doing.
“This is a great collaborative effort,” Holston said. “Through Healthy Communities, we will be able to use the RURAL study data to inform policy, systems, and environmental change strategies to increase access to healthy foods and physical activity in each community.”